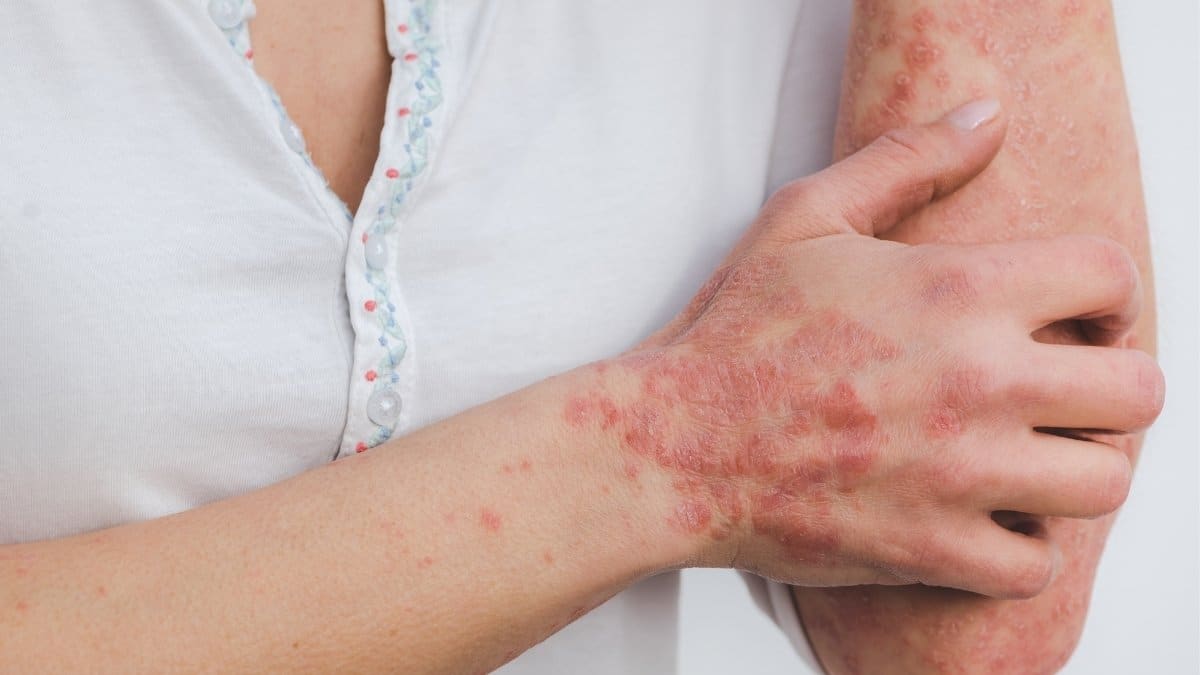
What Is Psoriasis?
Psoriasis is a skin disease that causes skin cells to multiply faster than usual (about ten times). It makes the skin accumulate into uneven red patches surrounded by white scales.
They can develop anywhere, although some of the most common sites of occurrence are- the scalp, knees, elbows, and lower back. Psoriasis is not infectious, which implies that a person with the condition cannot pass on the disease to others. Sometimes, it can happen between the members of the family.
Psoriasis can occur at any age but generally happens in early adulthood years. the condition usually remains limited to some areas of the body. Although, in severe cases, it can extend to cover several parts of the body.
What Are The Types Of Psoriasis?
Plaque Psoriasis
Plaque psoriasis is one of the most common types of psoriasis. About 8 in 10 people have this kind of psoriasis only. Sometimes, the doctor may also refer to it as “Psoriasis Vulgaris.”
The reason why the name plaque psoriasis is simple – It is because of the well-specified areas of bumpy red skin, which characterizes this form. These elevated red plaques have a silver-white, flaky buildup on top called scale that is composed of dead skin cells. With time, these scales loosen up and shed often.
What Are The Symptoms?
Plaque psoriasis causes bumpy and inflamed red skin covered with white-silvery scales. These patches may burn or itch. It can happen anywhere on the body, but generally pops up in the following regions:
- Scalp
- Face
- Knees
- Hands
- Feet
- Skin folds
- The outside of the elbow
What Are The Treatment Alternatives?
- Topical Treatments: This goes on your skin, and this is the first treatment your doctor will provide for plaque psoriasis.
- Phototherapy: It uses light, and that’s the reason it is called phototherapy. You can get it at your home or the doctor’s clinic having a phototherapy unit.
- Systemic Medications: If you have moderate to severe psoriasis, the doctor will recommend taking systemic medications, if no other treatment alternative for you. You can take them as a shot, IV, or only by mouth. Biologics also falls into this category alone, which targets specific parts of the immune system, and which has a significant role in the inflammatory process.
Guttate Psoriasis
This type of psoriasis is rare and accounts for only 2% of the total psoriasis cases. It usually starts with children or younger adults.
In guttate psoriasis, you will have small, pink, or red spots on your skin. The most common areas of occurrence include
- Scalp
- Trunk
- Thighs
- Upper arms
This type of psoriasis can go away in a couple of weeks, even without treatment. Although, some cases can take a severe form and demand proper treatment.
What Are The Symptoms?
It involves sudden flare-ups of symptoms. You will experience small, red marks that intensify and expand. They may remain in small patches or can even extend to cover large portions of the body.
Guttate psoriasis multitudes usually appear:
- Red or dark pink
- Small in size
- Separate from each other
- On the limbs or trunk
- Thinner than the kind of lesions involved in plaque psoriasis
What Are The Treatment Alternatives?
Most cases of guttate psoriasis cure on its own within 2-3 weeks. However, the doctor may suggest some kind of treatment to reduce the symptoms and avoid other infections in the body.
Medications
There are several over-the-counter medications available that can help treat itchy and flaky skin, as well as swelling and dryness. They include the following.
- Cortisone cream for swelling and itching
- Anti-dandruff shampoos for your scalp
- Moisturizers
- Lotions having cold tar to help calm your skin
- Prescription drugs with or without vitamin A
- If your cases of psoriasis are severe, the doctor may prescribe oral medications such as – corticosteroids, methotrexate, apremilast (otezla)
Phototherapy
One another treatment alternative you can consider is phototherapy. Your doctor will use intense a strong beam of ultraviolet radiation on your skin during this treatment. He may also provide certain medications to ensure your body reacts quickly to light. Sometimes, just stepping out of home and having sunlight exposure can be helpful.
Inverse Psoriasis
Inverse psoriasis is a condition in which red and inflamed lesions occur in the skin folds. It is sometimes also referred to as intertriginous psoriasis. These are the regions of the body where skin rubs against each other. The most common sites of occurrence include:
- Groin
- Armpits
- Under the breasts
- Skin folds around the buttocks or genitals
Some of the common triggers are:
- Sweating
- Friction
- Fungal infections
What Are The Symptoms?
- Patches of skin that are bright red, shiny, smooth, but are not scaly
- Symptoms that worsen with rubbing and sweating
What Are The Treatment Alternatives?
Topical Treatment
The topical creams are usually the first-line treatment alternative, which involves applying the cream over the affected site.
The motto of this treatment is to decrease the inflammation and other sorts of discomfort in these sensitive regions. Since the skin fold regions are susceptible, you must use the medications carefully.
Steroid creams are capable of reducing inflammation of the skin, but also can make your skin thinner and more sensitive. In case you are given a topical treatment, the doctor will continuously keep a check on your progress, and adjust the dosage if required.
The best time to take topical medications are:
- In the morning after you take a shower,
- And once again before bedtime
Infected Inverse Psoriasis Treatment
Inverse psoriasis makes you susceptible to yeast and fungal infections, and so your doctor can dilute the medication and add some anti-yeast and antifungal medications.
Phototherapy
Phototherapy can also be useful for moderate to severe psoriasis. In this, UVB rays are utilized to decelerate the growth of skin cells in some people.
This therapy utilizes a lightbox that produces artificial UVB rays for a certain specified amount of time in each session.
Phototherapy can first worsen your symptoms before making it better. Keep your doctor informed about the way you feel and the symptoms you experience.
Systemic Drugs
Systemic drugs can also be given for some patients with inverse psoriasis.
Pustular Psoriasis
This type of psoriasis is rare and usually occurs in adults. You can have fluid-filled bumps or blisters surrounded by red skin. Pustular psoriasis may appear as if they are infectious, but are certainly not.
Pustular psoriasis may appear on one part of the body, such as feet or hands. In rare cases, it can even stretch to many parts of the body as well. In cases where it affects many body parts, it is called “generalized pustular psoriasis.” It can sometimes become severe, so seek adequate medical assistance.
Common triggers are listed below:
- Emotional stress
- Pregnancy
- Infection
- Exposure to certain chemicals
- Getting excessive ultraviolet radiation without a sunscreen
- Sudden withdrawal of topical medicine or systemic drugs, especially steroids
What Are The Symptoms?
Pustular psoriasis symptoms include the following:
- Fast heart rate
- Fever
- Chills
- Nausea
- Muscle weakness
What Are The Treatment Alternatives?
The right treatment depends on the type of psoriasis you have and how severe it is. Sometimes, it requires several approaches or a combination of many different drugs to find the most effective treatment for your condition.
The doctor will first prescribe you some ointments as they possess the ability to reduce the inflammation and soothe your skin. Both artificial and natural ultraviolet light can help treat many different types of psoriasis, including pustular psoriasis. One another alternative is the PUVA treatment that involves a combination of UV light and medication that can make your skin even more sensitive towards it.
Your doctor may suggest taking the following medications:
- Cyclosporine
- Methotrexate
- Acitretin
- TNF alpha-blockers, including adalimumab (Humira), infliximab (Remicade), and etanercept (Enbrel)
- Oral psoralen plus ultraviolet A light
- Interleukin-12/23 inhibitors, including ustekinumab (Stelara)
Interleukin-12/23 inhibitors and TNF alpha blockers belong to a potent class of drugs called biologics.
If you’ve generalized pustular psoriasis, you need to take measures to prevent infection and check dehydration.
Also Read: Psoriasis: Know The Types, Symptoms & Treatment
Erythrodermic Psoriasis
Erythrodermic Psoriasis is one of the rarest, but the most dangerous form of psoriasis. It affects several parts of the body and can lead to widespread, fiery skin that looks as if it is burnt.
What Are The Symptoms?
The signs and symptoms of erythrodermic psoriasis are usually very intense. Some of the most common ones include the following:
- Pustules or blisters
- Severe itching
- Intense pain
- Severe skin redness that extends to many parts of the body
- Burnt looking skin
- Skin shedding that occurs in large sheets rather than smaller flakes or scales
- Increased heart rate
- Fluctuations in body temperature
Most people with erythrodermic psoriasis will experience these symptoms during flare-ups. The condition can completely transform the chemistry of your body, and you can also experience some other symptoms, including
- Joint pain
- Chills or fever
- Swelling, especially around the ankles
Some of the most prevalent triggers for erythrodermic psoriasis are listed below:
- Emotional stress
- Infection
- Severe sunburn
- Alcoholism
- Use of systemic drugs
- Sudden withdrawal of systemic medications
What Are The Treatment Alternatives?
Medications
Few oral medications can help treat your erythrodermic psoriasis. It includes:
- golimumab (Simponi)
- ixekizumab (Taltz)
- etanercept (Enbrel)
- adalimumab (Humira)
- infliximab, a drug used to treat autoimmune diseases
- acitretin (Soriatane)
- cyclosporine, an anti-rejection drug that dampens the immune response that causes psoriasis
- methotrexate, a cancer treatment that can help treat erythrodermic psoriasis
All these medications can be helpful but can cause severe side effects. For this reason, stay in contact with your doctor whenever you take these medications.
Other Treatments
For the most appropriate treatment for any kind of psoriasis, you need to consult a dermatologist. Your doctor may prescribe you a combination of topical and oral medication. Combining different drugs may be more effective than the single drug alone.
Sometimes, you may also have to take some pain relievers to ease your discomfort and even some medication that can help you sleep. Some people also receive antibiotics to get rid of their infection, and some medicines to get relief from their itchiness.
Nail Psoriasis
Nail psoriasis accounts for nearly half of the total psoriasis cases. The condition is even more prevalent in people with psoriatic arthritis, which affects the joints.
Nail psoriasis changes the way your fingernails and toenails appear. They may get thickened, create pin-prick holes, and transform the shape or color of the nails. You may also feel that your nails have become tender and hurt.
What Are The Symptoms?
- The nails may turn pale, green, or brown. They may also have small white or red spots beneath.
- You may also get grooves or ridges in your nails, or pitting on the surface of the nails.
- Chalky, white material can accumulate underneath your nail, making it lift away from the skin. It can be excruciating.
- The nail may loosen and separate from the nail bed.
- About one-third of people with nail psoriasis get a fungal infection as well, which can make your nail thick. The nails may also get brittle and fall off.
Some of the symptoms can make it very difficult for you to move your fingers. You may also experience pain and tenderness of the nails. All of these changes in nails can make it challenging to perform daily activities.
What Are The Treatment Alternatives?
You can take the same medications for nail psoriasis as it is recommended for other types of psoriasis. Some other treatment alternatives are listed below:
Medicine which you can apply directly on your nails: To treat nail psoriasis, your doctor may recommend taking a corticosteroid, retinoid creams, or vitamin D that you can use on your nails and cuticles every day.
If you have thick nails, the applied medication can take quite a long time to get inside. You can use some gels or ointments containing urea that can help make them thin.
Your doctor may also order a nail lacquer that not only hydrates them but also can strengthen them. You can apply it to your nails in the same way nail polish is applied.
Corticosteroid injections: These injections are put under the surface of your nails every 2-9 months. The doctor will first numb the site or make use of a nerve block to lower the pain.
Scalp Psoriasis
Scalp psoriasis is a common skin disorder that makes inflated, reddish, and scaly patches on your scalp. It can emerge as a single patch, or many small patches that can cover a large part or even the entire scalp. It can also spread to the back of your neck, forehead, and inside ears.
What Are The Symptoms?
Mild scalp psoriasis only involves fine, slight scaling. However, a severe to moderate scalp psoriasis can cause the following:
- Scaly, red, bumpy patches
- Silvery, white scaly patches
- Itching
- Dry scalp
- Dandruff-like flaking
- Hair loss
- Burning or soreness
Note that there is no direct link between scalp psoriasis and hair loss. Although frequent scratching, picking at the scaly spots, stress, and harsh treatments that carry along with the condition can be the reason for your temporary hair loss. Luckily, hair growth becomes normal after the skin clears.
What Are The Treatment Alternatives?
Topical Medications
Topical medications such as cold tar, salicylic acid, and clobetasol propionate can be helpful. You can directly apply them as a cream or shampoo on the affected regions.
Biologic drugs
These are the newly discovered drugs that target certain specific molecules in the immune system.
One example of biologic drugs is brodalumab, having the brand name SILIQ. FDA approves this drug for the treatment of psoriasis. But brodalumab can cause many adverse effects. Also, it comes with a warning of increased suicidal thinking or behavior. Other alternatives include:
- ixekizumab (brand name: TALTZ)
- secukinumab (brand name: Cosentyx)
These drugs target selective cells in the immune system that causes an increase in the production of cells. As these drugs decrease the immune system response, they can make the person more susceptible to different infections. So, the doctor will always monitor the person taking these drugs.
If you’ve latent tuberculosis, frequent or recurrent infection, inform your doctor before taking any of the biologic drugs.
How Is Psoriasis Diagnosed?
The doctor can take the following tests to confirm the diagnosis of psoriasis:
Physical Examination
In most cases, the doctor can suspect psoriasis by appearance alone. The examination can be carried out with the naked eye or a lighted magnifying tool called dermatoscope. Several reports of flare-ups in which the symptoms develop spontaneously and also resolve quickly can also be beneficial in confirming the diagnosis.
Medical history also plays a crucial role. It helps reveal the conditions that place you at an elevated risk for psoriasis. Some of the common examples include:
- A family history with psoriasis or other conditions
- A recent strep throat infection
- A recent immunization
- An immunosuppressive condition such as psoriasis
- Other autoimmune conditions
Labs And Tests
In some cases, a rash can appear different than usual; in such a case, a closer examination is required. A microscopic level of tissue examination, as in the case of skin biopsy, may be helpful.
Sources:
Tags: Psoriasis treatments, Psoriasis symptoms, Psoriasis types