Angina Pectoris Anti-Anginals
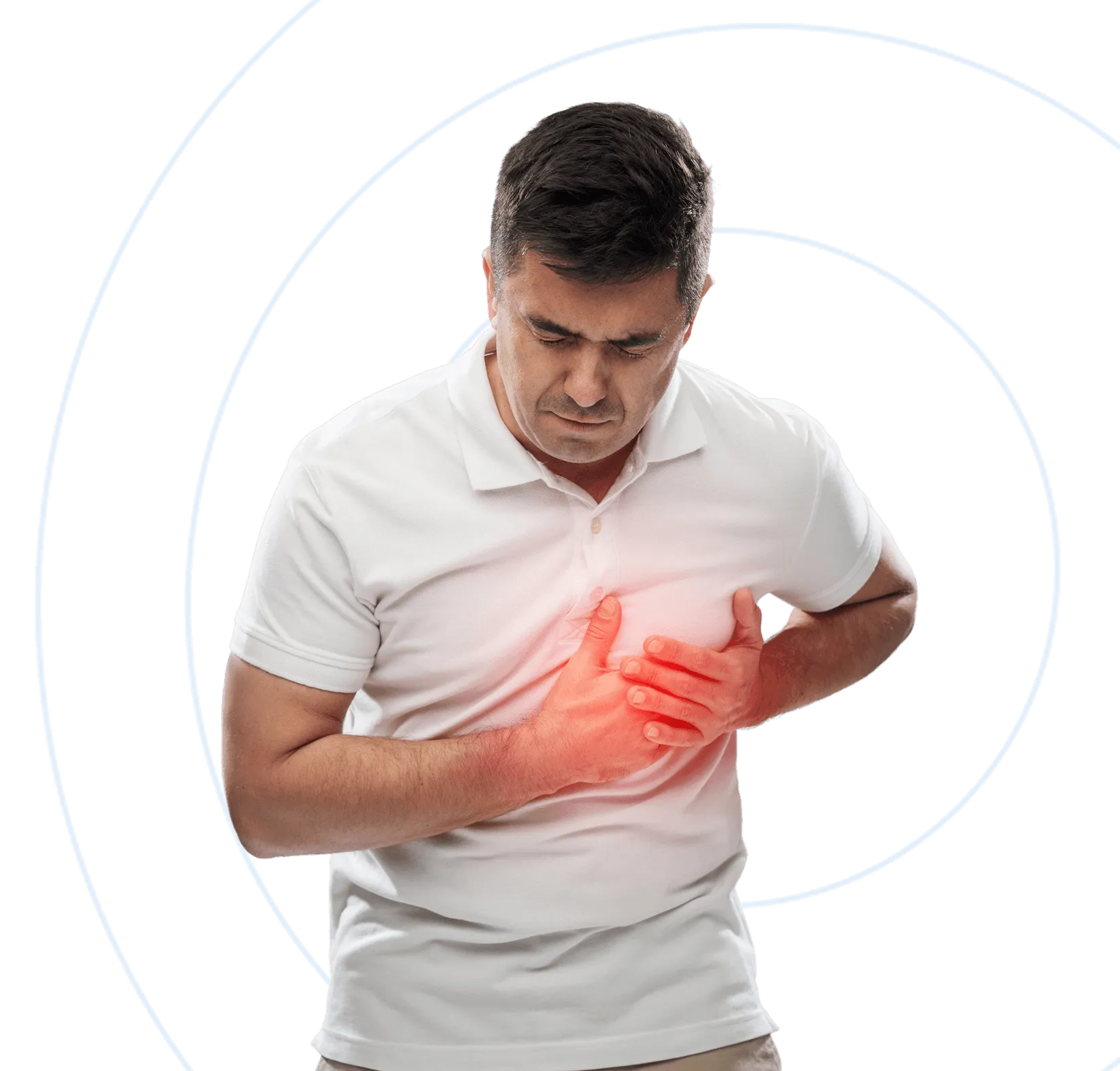
Angina Pectoris
Angina Pectoris is the medical jargon applied to Chest Pain. Angina means pain (intense pain) and Pectoris means chest. In order to avoid confusion, it is used only for chest pain due to cardiac causes specifically stable angina.
Symptoms:
Chest pain, palpitations, sweating and anxiety following physical exertion. It would be relieved after some time or at rest.
Precipitating Factors:
Any activity that demands the heart to work harder results in the precipitation of an episode of angina. Some of the factors are as follows:
Common Factors:
- Physical exertion
- Cold Exposure
- Heavy meals
- Intense emotion
- Sexual intercourse and orgasms
- Straining hard
Uncommon Factors:
- Lying flat(decubitus angina)
-
Vivid dreams(nocturnal angina)
-
Cardiac Features causing Angina are:
-
Any factors that cause disparity between the demand and supply of heart muscle blood supply and work results in angina pectoris.
Factors influencing myocardial oxygen supply and demand:
-
Cardiac Work
-
Heartrate
-
BP
-
Myocardial contractility
-
Left ventricular hypertrophy
-
Valve disease e.g.aortic stenosis
Investigations:
Evaluation of angina involves putting the patient under stress and identify if an angina can be precipitated. Following are some of the possible investigations:
- Resting ECG– this would serve as the reference ECG or the reference status of the heart when the patient is asymptomatic and comfortable.
- Exercise ECG - An exercise tolerance test (ETT) is usually performed using a standard treadmill or bicycle ergometer while monitoring the patient’s ECG, BP and general condition. Specific ECG changes suggestive of Angina pectoris may be identified in the ECG. Exercise testing is also a useful means of assessing the severity of coronary disease and identifying high-risk individuals. For example, the amount of exercise that can be tolerated and the extent and degree of any ECG segment change provide a useful guide to the likely extent of coronary disease.
- Myocardial perfusion scanning- This may be helpful in the evaluation of patients with an equivocal or uninterpretable exercise test and those who are unable to exercise. It entails obtaining small pictures of the myocardium at rest and during stress (either exercise testing or pharmacological stress, such as a controlled infusion of cardiotonic agents), after the administration of an intravenous radioactive isotope, such as 99 technetium tetrofosmin. Thallium and tetrofosmin are taken up by viable perfused myocardium. A perfusion defect present during stress but not at rest provides evidence of reversible myocardial ischaemia suggestive of Angina Pectoris or any other kind of angina whereas a persistent perfusion defect seen during both phases of the study is usually indicative of previous MI.
- Stress echocardiography- This is an alternative to myocardial perfusion scanning and can achieve similar predictive accuracy. It uses transthoracic echocardiography to identify ischaemic segments of myocardium and areas of infarction. The former characteristically exhibits reversible defects in Stress echocardiography. Echocardiography uses a technique similar to ultrasonography where sound waves are sent using a probe and the reflected waves are collected to form an image and identify the blood flow to those areas.
- Coronary angiography- This is a straightforward measure to identify any narrowing of the coronary arteries. Coronary arteries are the arteries supplying the heart muscles. When there is a filling defect indicative of atherosclerotic plaque in the coronary arteries, some kind of coronary artery disease (CAD) like stable angina, unstable angina or mycocardial ischemia or infarction may be the diagnosis.
Assessment of risk in Angina Pectoris:
High risk:
-
Post-infarct angina
-
Pooreffort tolerance
-
Ischaemia at low workload
-
Leftmainor three vessel disease
-
Poor LV function
Low risk:
-
Predictable exertional angina
-
Good effort tolerance
-
Ischaemia only at high workload
-
Single- vessel or two -vessel disease
-
Good LV function
Management of Angina Pectoris:
General Measures:
-
Careful assessment of the likely extent and severity of arterial disease
-
The identification and control of risk factors such as smoking, hypertension and hyperlipidaemia
-
The use of measures to control symptoms
-
The identification of high-risk patients for treatment to improve life expectancy.
Medical Management:
-
Antiplatelet drugs like aspirin, clopidogrel which prevent the aggregation of platelets and hence the formation of any thrombus or embolus is prevented.
-
Antianginal drugs like nitrates, beta blockers, calcium channel blockers, nicorandil, ivabradine. These drugs act by either increasing the blood flow through the coronary arteries or decreasing the work load of the heart. Both of these help in Angina Pectoris.
Invasive Management:
- Percutaneous coronary intervention (PCI)- Percutaneous coronary intervention (PCI) is performed by passing a fine guide wire across a coronary stenosis under radiographic control and using it to position a balloon, which is then inflated to dilate the stenosis. A coronary stent is a piece of coated metallic ‘scaffolding’ that can be deployed on a balloon and used to maximise and maintain dilatation of a narrowed vessel. The routine use of stents in appropriate vessels reduces both acute complications and the incidence of clinically important recurrence of Angina Pectoris. PCI provides an effective symptomatic treatment but definitive evidence that it improves survival in patients with chronic stable angina is lacking. It is mainly used in single- or two-vessel disease. Stenoses in bypass grafts can be dilated, as well as those in the native coronary arteries. The technique is often used to provide palliative therapy for patients with recurrent angina after CABG. Coronary surgery is usually the preferred option in patients with three-vessel or left main stem disease, although recent trials have demonstrated that PCI is also feasible in such patients.The main acute complications of PCI are occlusion of the target vessel or a side branch by a thrombus or a loose flap of intima (coronary artery dissection), and consequent myocardial damage. This occurs in about 2–5% of procedures and can often be corrected by deploying a stent; however, emergency CABG is sometimes required. Minor myocardial damage, as indicated by elevation of sensitive intracellular markers, occursin up to 10% of cases. The main long-term complication of PCI is re-stenosis, in up to one-third of cases. This is due to a combination of elastic recoil and smooth muscle proliferation (neo-intimal hyperplasia) and tends to occur within 3 months. Stenting substantially reduces the risk of re-stenosis, probably because it allows the operator to achieve more complete dilatation in the first place. Drug-eluting stents reduce this risk even further by allowing an antiproliferative drug, e.g. sirolimus or paclitaxel, to elute slowly from the coating and prevent neo-intimal hyperplasia and in-stent re-stenosis. There is an increased risk of late stent thrombosis with drug-eluting stents, although the absolute risk is small (< 0.5%). Recurrent angina (affecting up to 15–20% of patients receiving an intracoronary stent at 6 months) may require further PCI or bypass grafting. The risk of complications and the likely success of the procedure are closely related to the morphology of the stenoses, the experience of the operator and the presence of important comorbidity, e.g. diabetes, peripheral arterial disease. A good outcome is less likely if the target lesion is complex, long, eccentric or calcified, lies on a bend or within a tortuous vessel, involves a branch or contains acute thrombus. In combination with aspirin and heparin, adjunctive therapy with potent platelet inhibitors, such as clopidogrel or glycoprotein IIb/IIIa receptor antagonists, improves the outcome of PCI, with lower short- and long-term rates of death and MI.
- Coronary artery bypass graft- The internal mammary arteries, radial arteries or reversed segments of the patient’s own saphenous vein can be used to bypass coronary artery stenoses. This usually involves major surgery under cardiopulmonary bypass but, in some cases, grafts can be applied to the beating heart: ‘off-pump’ surgery. The operative mortality is approximately 1.5% but risks are higher in elderly patients, those with poor left ventricular function and those with significant comorbidity, such as renal failure. Approximately 90% of patients are free of angina 1 year after CABG surgery, but fewer than 60% of patients are asymptomatic after 5 or more years. Early postoperative angina is usually due to graft failure arising from technical problems during the operation, or poor ‘run-off’ due to disease in the distal native coronary vessels. Late recurrence of angina may be due to progressive disease in the native coronary arteries or graft degeneration. Fewer than 50% of vein grafts are patent 10 years after surgery. However, arterial grafts have a much better long-term patency rate, with more than 80% of internal mammary artery grafts patent at 10 years. This has led many surgeons to consider total arterial revascularisation during CABG surgery. Aspirin (75–150 mg daily) and clopidogrel (75 mg daily) both improve graft patency, and one or other should be prescribed indefinitely, if well tolerated. Intensive lipid lowering therapy slows the progression of disease in the native coronary arteries and bypass grafts, and reduces clinical cardiovascular events. There is substantial excess cardiovascular morbidity and mortality in patients who continue to smoke after bypass grafting. Persistent smokers are twice as likely to die in the 10 years following surgery than those who give up at surgery. CABG improves survival in symptomatic patients with left main stem stenosis or three-vessel coronary disease or two-vessel disease involving theproximal LAD coronary artery. Improvement in survival is most marked in those with impaired left ventricular function or positive stress testing prior to surgery and in those who have undergone left internal mammary artery grafting. Neurological complications are common, with a 1–5% risk of perioperative stroke. Between 30% and 80% of patients develop short-term cognitive impairment that typically resolves within 6 months. There are also reports of long-term cognitive decline that may be evident in more than 30% of patients at 5 years.
Prognosis of Angina Pectoris:
The prognosis of coronary artery disease is related to the number of diseased vessels and the degree of left ventricular dysfunction. A patient with single-vessel disease and good left ventricular function has an excellent outlook (5-year survival > 90%), whereas a patient with severe left ventricular dysfunction and extensive three-vessel disease has a poor prognosis (5-year survival < 30%) without revascularisation. Spon-taneous symptomatic improvement due to the develop-ment of collateral vessels is common.
Lifestyle Modifications:
- Do not smoke
-
Aim for ideal bodyweight
-
Take regular exercise(exercise upto, but not beyond, the point of chest discomfort is beneficial and may promote collateral vessels)
-
Avoid severe unaccustomed exertion, and vigorous exercise after a heavy meal or in very cold weather
-
Take sublingual nitrate before undertaking exertion that may induce angina.